In Vitro Fertilization: Biology, Procedure & Ethics
A comprehensive introduction to IVF for biomedical students, covering clinical procedures, success rates, hormonal regulation, and future AI technologies.
A Scientific Introduction for First-Year Biomedical Sciences Students
Department of Biomedical Sciences | 2026
Presentation Overview
Definition & Purpose of IVF
Understanding the core concepts and primary clinical goals
Reproductive Biology Background
Key biological mechanics underlying human reproduction
Step-by-Step IVF Procedure
Detailed progression through clinical and laboratory steps
Success Rates & Influencing Factors
Analysis of clinical outcomes and critical demographic variables
Risks & Limitations
Potential medical complications and procedural boundaries
Ethical & Societal Considerations
Examining the moral implications and broader social impact
Future Developments in IVF
Emerging technologies and innovations shaping tomorrow's treatments
10–15 min presentation
What is IVF?
In Vitro Fertilization (IVF) is an assisted reproductive technology (ART) in which oocytes are fertilized by sperm outside the body, in a controlled laboratory environment, before the resulting embryo is transferred to the uterus.
01 — Definition & Purpose
Why is IVF Used?
Common Causes of Infertility
Female Factor
Male Factor
Other Indications
<li style="margin-bottom: 16px; padding-left: 8px;">Blocked or damaged fallopian tubes</li><li style="margin-bottom: 16px; padding-left: 8px;">Endometriosis</li><li style="margin-bottom: 16px; padding-left: 8px;">Polycystic Ovary Syndrome (PCOS)</li><li style="margin-bottom: 16px; padding-left: 8px;">Diminished ovarian reserve</li><li style="margin-bottom: 16px; padding-left: 8px;">Unexplained ovulatory dysfunction</li>
<li style="margin-bottom: 16px; padding-left: 8px;">Low sperm count (oligospermia)</li><li style="margin-bottom: 16px; padding-left: 8px;">Poor sperm motility (asthenospermia)</li><li style="margin-bottom: 16px; padding-left: 8px;">Abnormal morphology (teratospermia)</li><li style="margin-bottom: 16px; padding-left: 8px;">Azoospermia (no sperm in ejaculate)</li>
<li style="margin-bottom: 16px; padding-left: 8px;">Unexplained infertility</li><li style="margin-bottom: 16px; padding-left: 8px;">Genetic disease screening (PGT)</li><li style="margin-bottom: 16px; padding-left: 8px;">Same-sex couples / single parents</li><li style="margin-bottom: 16px; padding-left: 8px;">Fertility preservation (cancer patients)</li>
<span style="color: #00C9B8; font-weight: 700; font-size: 30px; margin-right: 8px;">1 in 6</span> couples worldwide experience infertility <span style="font-size: 20px; color: #A0B0C0; margin-left: 10px; opacity: 0.8;">(WHO, 2023)</span>
02 — REPRODUCTIVE BIOLOGY BACKGROUND
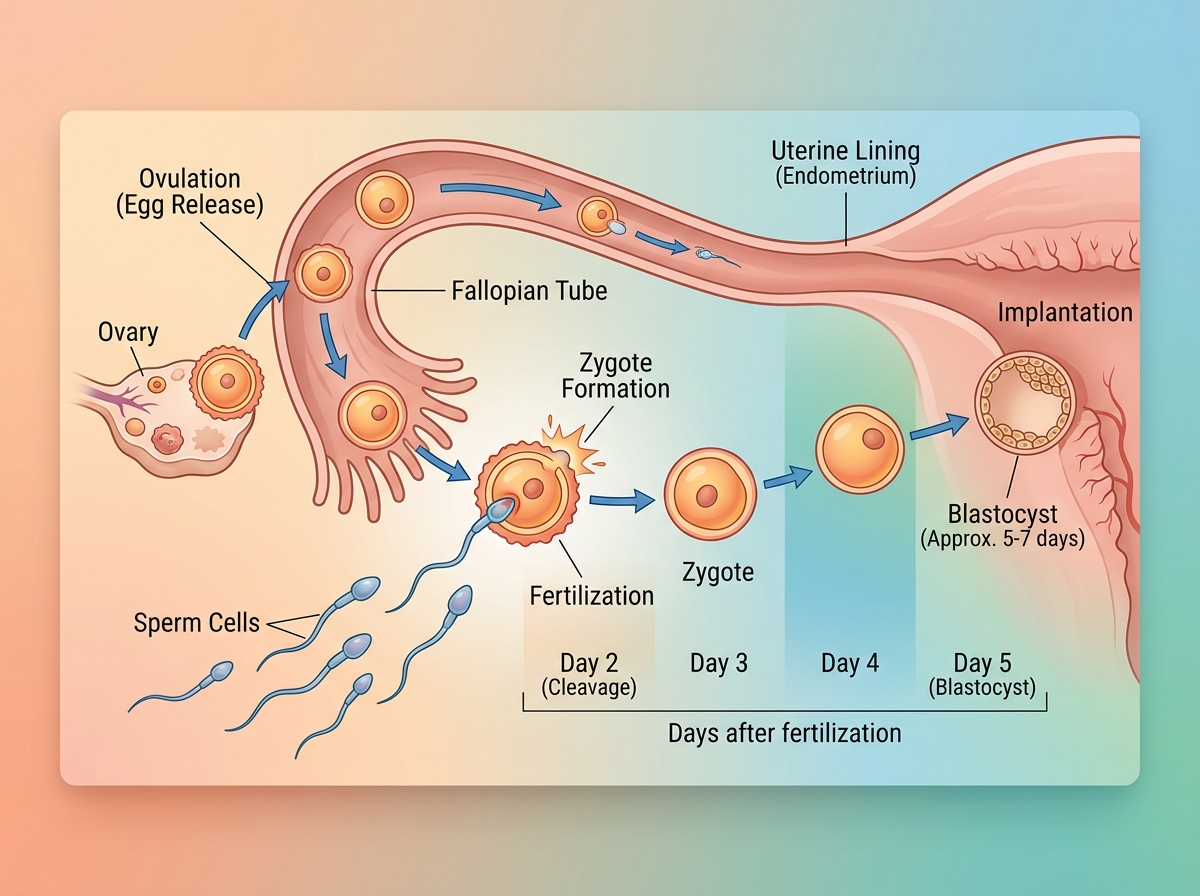
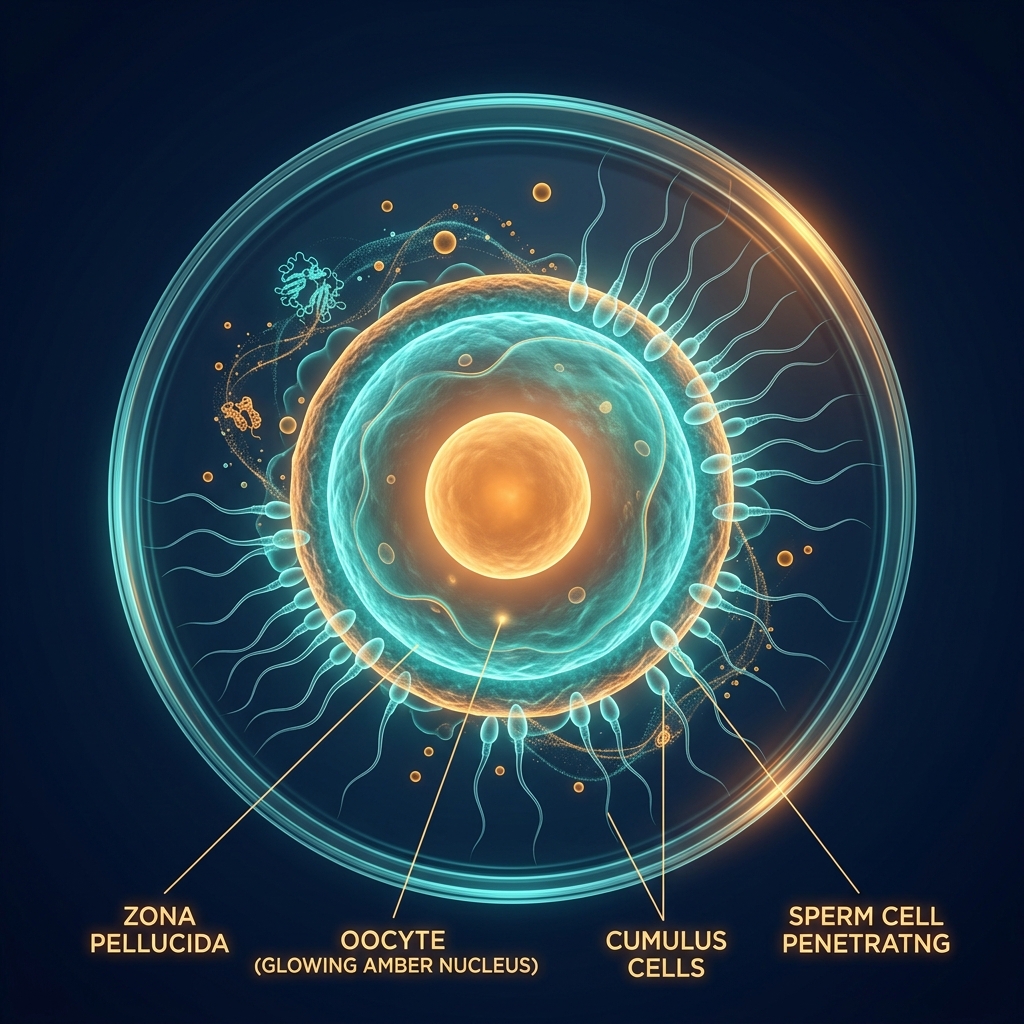
The Natural Fertilization Process
Hormonal Regulation of the Menstrual Cycle
Stimulates follicular development in the ovary
Triggers ovulation; targets the dominant follicle
Promotes endometrial proliferation; triggers LH surge
Maintains endometrium for implantation
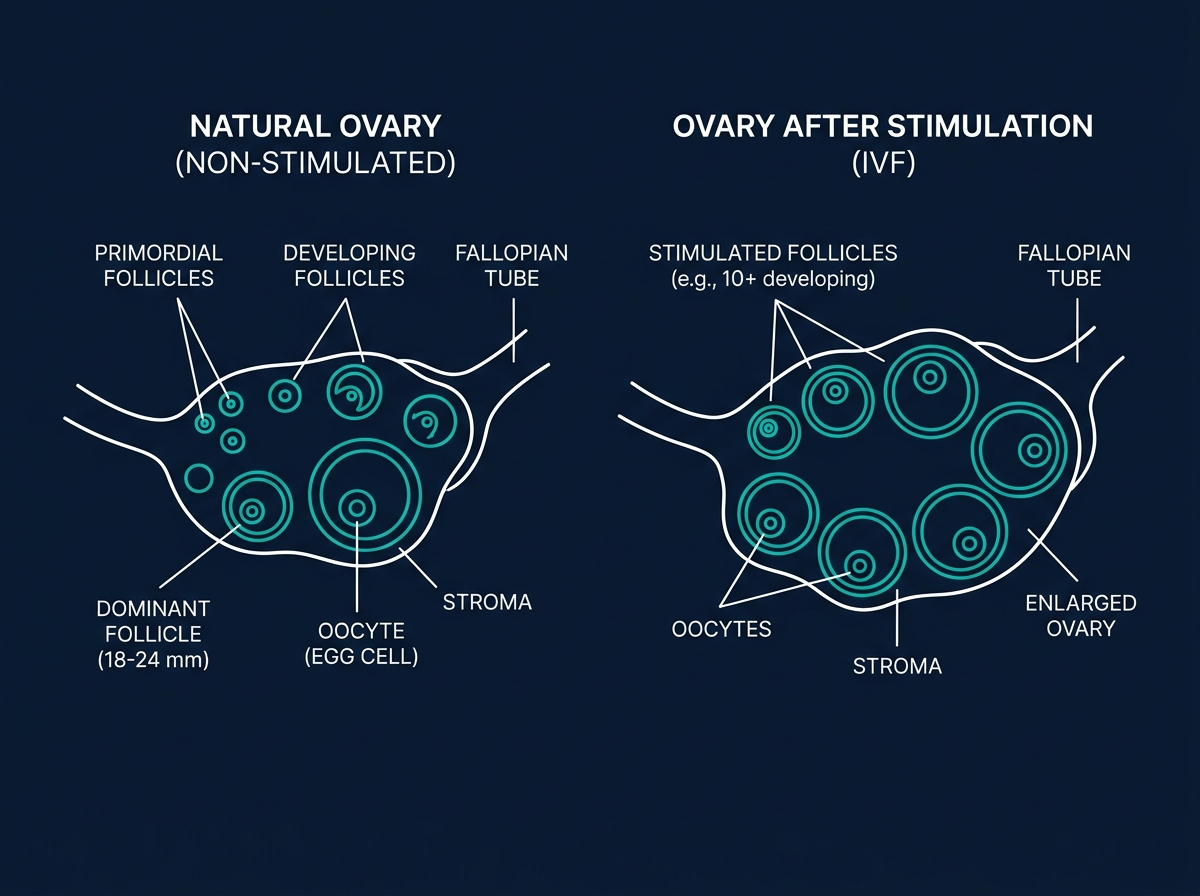
IVF protocols use exogenous gonadotropins (FSH/LH) to stimulate multiple follicle development.
Ovarian Stimulation
Gonadotropin injections stimulate multiple follicle growth
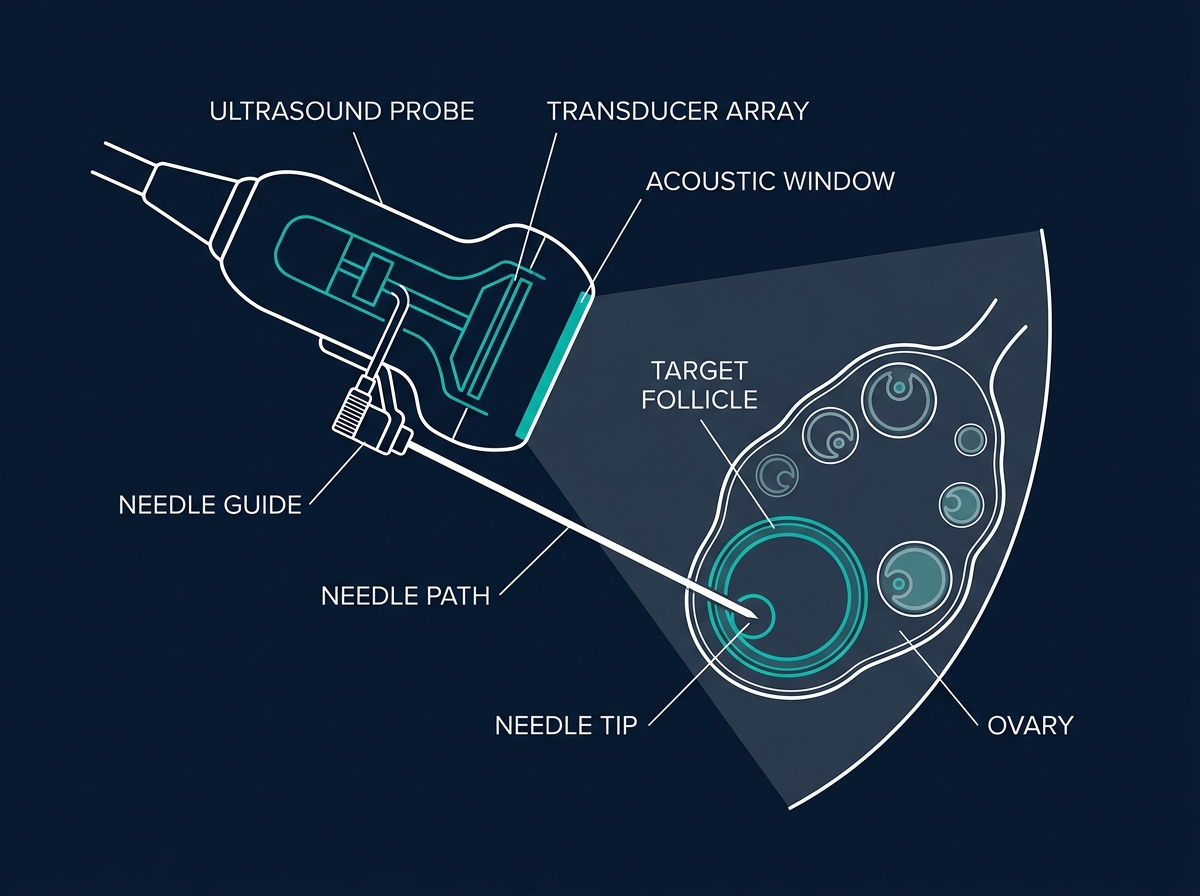
Oocyte Retrieval
Transvaginal ultrasound-guided follicular aspiration
Fertilization
Standard IVF or ICSI in laboratory
Embryo Culture
Embryos cultured 3–5 days to blastocyst stage
Embryo Transfer
Selected embryo placed into the uterus
Pregnancy Testing
βhCG blood test 10–14 days post-transfer
Department of Biomedical Sciences | Core Procedure Overview
03 — Step-by-Step IVF Procedure
03 — Step-by-Step IVF Procedure
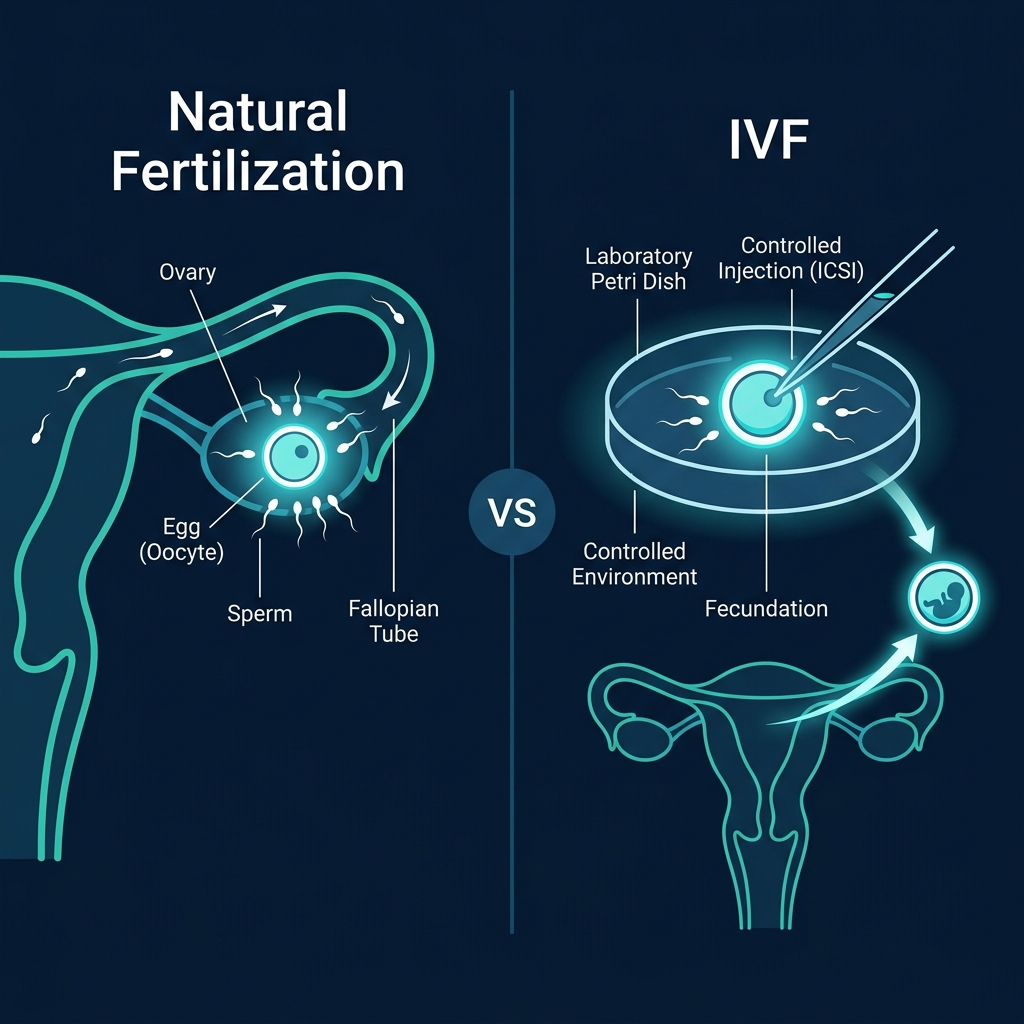
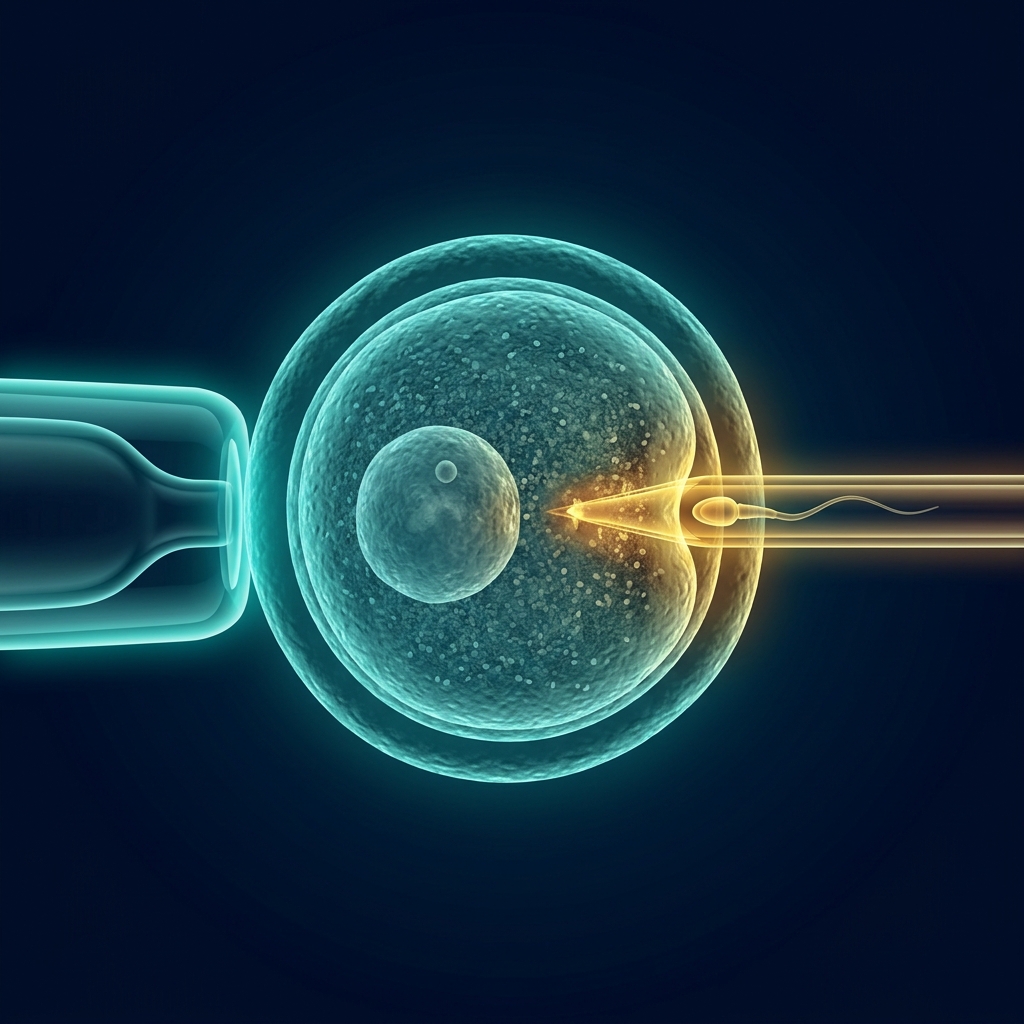
Step 3: Fertilization —
Standard IVF vs. ICSI
Both methods: fertilization confirmed 16–18h later by presence of two pronuclei (2PN)
03 — Step-by-Step IVF Procedure
Steps 4 & 5: Embryo Culture & Transfer
<div style="display: flex; align-items: flex-start; gap: 15px;"><div style="width: 8px; height: 8px; border-radius: 50%; background-color: #00C9B8; margin-top: 8px; flex-shrink: 0; box-shadow: 0 0 8px rgba(0,201,184,0.6);"></div><p style="color: #E2E8F0; font-size: 19px; line-height: 1.5; margin: 0;">Embryos cultured in specialized <strong style="color: #FFFFFF;">CO₂ incubators at 37°C</strong> in sequential culture media</p></div><div style="display: flex; align-items: flex-start; gap: 15px;"><div style="width: 8px; height: 8px; border-radius: 50%; background-color: #00C9B8; margin-top: 8px; flex-shrink: 0; box-shadow: 0 0 8px rgba(0,201,184,0.6);"></div><p style="color: #E2E8F0; font-size: 19px; line-height: 1.5; margin: 0;"><strong style="color: #FFFFFF;">Blastocyst transfer (Day 5) preferred</strong> — higher implantation rates vs. Day 3 cleavage transfer</p></div><div style="display: flex; align-items: flex-start; gap: 15px;"><div style="width: 8px; height: 8px; border-radius: 50%; background-color: #00C9B8; margin-top: 8px; flex-shrink: 0; box-shadow: 0 0 8px rgba(0,201,184,0.6);"></div><p style="color: #E2E8F0; font-size: 19px; line-height: 1.5; margin: 0;"><strong style="color: #FFFFFF;">Embryo grading:</strong> morphological assessment of ICM quality and trophectoderm cell layer</p></div><div style="display: flex; align-items: flex-start; gap: 15px;"><div style="width: 8px; height: 8px; border-radius: 50%; background-color: #00C9B8; margin-top: 8px; flex-shrink: 0; box-shadow: 0 0 8px rgba(0,201,184,0.6);"></div><p style="color: #E2E8F0; font-size: 19px; line-height: 1.5; margin: 0;">Surplus viable embryos <strong style="color: #FFFFFF;">vitrified (cryopreserved)</strong> for future family building</p></div>
<div style="display: flex; align-items: flex-start; gap: 15px;"><div style="width: 8px; height: 8px; border-radius: 50%; background-color: #00C9B8; margin-top: 9px; flex-shrink: 0; box-shadow: 0 0 8px rgba(0,201,184,0.6);"></div><p style="color: #E2E8F0; font-size: 20px; line-height: 1.5; margin: 0;">Ultrasound-guided procedure using a highly specialized, <strong style="color: #FFFFFF;">soft transfer catheter</strong> through the cervix</p></div><div style="display: flex; align-items: flex-start; gap: 15px;"><div style="width: 8px; height: 8px; border-radius: 50%; background-color: #00C9B8; margin-top: 9px; flex-shrink: 0; box-shadow: 0 0 8px rgba(0,201,184,0.6);"></div><p style="color: #E2E8F0; font-size: 20px; line-height: 1.5; margin: 0;"><strong style="color: #FFFFFF;">Quick and non-invasive:</strong> Usually painless; takes 5–10 minutes; no anesthesia required</p></div><div style="display: flex; align-items: flex-start; gap: 15px;"><div style="width: 8px; height: 8px; border-radius: 50%; background-color: #00C9B8; margin-top: 9px; flex-shrink: 0; box-shadow: 0 0 8px rgba(0,201,184,0.6);"></div><p style="color: #E2E8F0; font-size: 20px; line-height: 1.5; margin: 0;"><strong style="color: #FFFFFF;">Luteal phase support:</strong> Progesterone supplementation (vaginal/IM) administered for 2 weeks post-transfer to prepare the uterine lining</p></div>
04 — Success Rates & Influencing Factors
Live Birth Rate per IVF Cycle by Age
Age is the single strongest predictor of IVF success
Source: HFEA National Statistics (2022)
Embryo Quality
Blastocyst morphology grade, euploidy status (PGT-A)
Ovarian Reserve
AMH levels, antral follicle count (AFC)
Sperm Parameters
Count, motility, morphology, DNA fragmentation index
Lifestyle Factors
BMI, smoking, alcohol, stress — all independently affect outcomes
Clinical Variables
Endometrial thickness ≥7mm, uterine pathology, protocol choice
05 — Risks & Limitations
Risks & Limitations of IVF
Embryo Status & Selection
Moral and legal status of the human embryo. Pre-implantation genetic testing (PGT) raises debates around "designer babies" and disability discrimination.
Surplus Embryo Storage
Unused embryos may be frozen for years. Decisions around donation, destruction, or research use are emotionally and ethically complex.
Accessibility & Equity
IVF remains financially inaccessible to many. Significant disparities exist by income, geography, ethnicity, and marital status in access to treatment.
Legal Frameworks
Legislation varies globally. UK: HFEA 1990 regulates IVF. Some countries ban embryo donation, surrogacy, or genetic screening entirely.
Gamete Donation
Donor sperm/egg raises questions of donor anonymity (now removed in UK since 2005), donor-conceived identity, and family structure definition.
Cultural & Religious Perspectives
IVF is prohibited or restricted in some religious traditions (e.g., certain Catholic teachings). Cultural attitudes to infertility and ART vary significantly worldwide.
"Science provides the tools; society must decide how to use them responsibly."
07 — Future Developments
Future Developments in IVF
Advanced Embryo Screening
Preimplantation Genetic Testing for Aneuploidies (PGT-A): selects euploid embryos → higher implantation, lower miscarriage
Non-invasive PGT (niPGT): analysis of spent culture media instead of embryo biopsy — preserves embryo integrity
AI-powered embryo morphokinetic grading using time-lapse imaging (EmbryoScope)
Mitochondrial DNA copy number as viability marker
Cryopreservation Advances
Vitrification (ultra-rapid freezing) now standard: >95% embryo survival vs. ~75% slow freezing
Ovarian tissue cryopreservation: restore fertility in cancer survivors
Oocyte banking for social fertility preservation
Freeze-all cycles: improved endometrial receptivity in fresh-cycle OHSS risk patients
Artificial intelligence predicting optimal warming protocols
Emerging Technologies
In vitro gametogenesis (IVG): deriving eggs/sperm from induced pluripotent stem cells (iPSCs) — could revolutionize infertility treatment
Uterine microbiome analysis for implantation optimization
Mitochondrial replacement therapy (MRT) for prevention of mitochondrial disease
Automated microfluidic ICSI systems
Womb-on-a-chip technology for embryo culture optimization
The future of IVF lies at the intersection of genetics, AI, and stem cell biology.
Conclusion
Key Take-Home Messages
IVF is a multi-step ART procedure that bypasses natural fertilization to help individuals and couples with infertility achieve pregnancy.
The procedure is underpinned by reproductive endocrinology — gonadotropin stimulation, oocyte maturation, and precise embryological techniques.
Success rates are strongly age-dependent and influenced by embryo quality, ovarian reserve, and lifestyle — live birth rates decline sharply after age 38.
IVF carries real medical, psychological, and financial risks — responsible clinical practice and informed consent are essential.
Rapid advances in PGT, AI-assisted selection, vitrification, and stem cell biology will continue to transform the field — but ethical frameworks must evolve alongside the science.
Gardner, D.K. et al. (2018). Textbook of Assisted Reproductive Techniques. CRC Press.
HFEA (2022). Fertility Treatment 2022: Trends and Figures. Human Fertilisation & Embryology Authority.
Zegers-Hochschild, F. et al. (2017). ART Terminology. Human Reproduction, 32(9), 1786–1801.
WHO (2023). Infertility Prevalence Estimates. World Health Organization.
Thank you | Questions Welcome
- ivf
- reproductive-biology
- assisted-reproductive-technology
- biomedical-science
- embryology
- fertility-treatment