Understanding Elephantiasis: Lymphatic Filariasis Guide
Explore the causes, symptoms, and treatment of Elephantiasis (Lymphatic Filariasis). Learn about the Wuchereria bancrofti parasite and global elimination efforts.
INFECTIOUS DISEASE REPORT
ELEPHANTIASIS
Lymphatic Filariasis
A Neglected Tropical Disease caused by parasitic worms
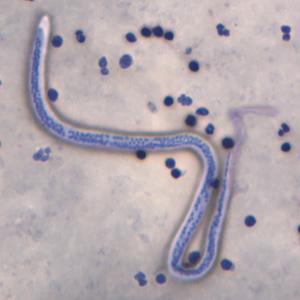
Wuchereria bancrofti microfilaria (×400)
Biology Infectious Disease Unit
01 — NAME OF DISEASE
Common Name
ELEPHANTIASIS
From Greek: 'elephas' (ἐλέφας) meaning elephant — referring to the thick, rough skin resembling elephant hide
Also called: Lymphedema, Tropical Elephantiasis
Scientific Name
Lymphatic Filariasis
Named after the filarial worms (Filarioidea) that infect the lymphatic system
ICD-10 Code: B74.0
The word 'Elephantiasis' was first used to describe the dramatic swelling and skin thickening that resembles an elephant's leg.
02 — THE PATHOGEN
Scientific Name
Wuchereria bancrofti
Named after Otto Wucherer & Joseph Bancroft, who discovered the worm in the 1800s
Brugia malayi, Brugia timori (less common)
Type of Pathogen
Parasitic Nematode
(Roundworm)
Size Range
Microfilaria:
280 μm long × 25 μm wide
Male adult worm:
40 mm long × 100 μm wide
Female adult worm:
60–100 mm long × 300 μm wide
L1 larvae:
124–250 μm
Female is 3× larger than male!
accounts for ~90% of all lymphatic filariasis cases globally. It is transmitted by mosquito bite.
03 — PATHOGEN STRUCTURE
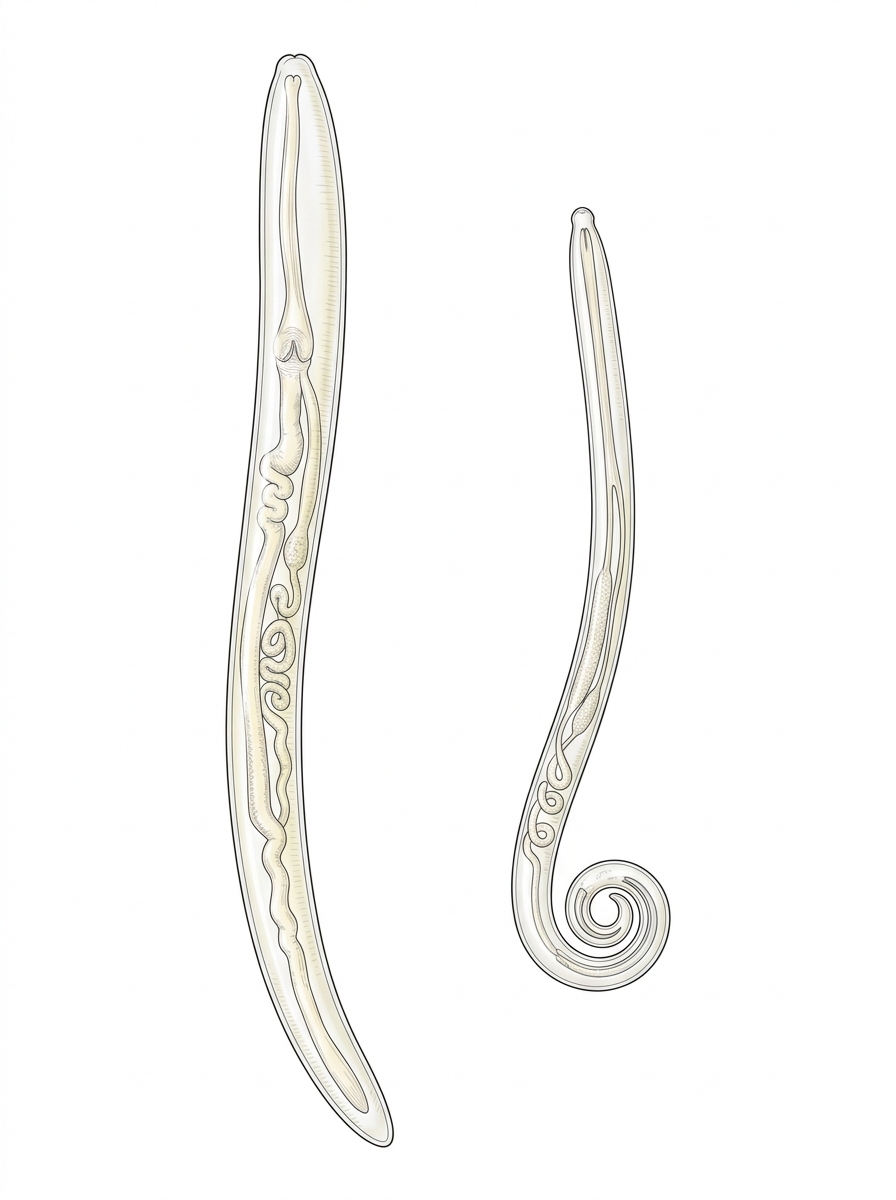
External Structure
Internal Structure
Microfilaria Stage
Adult worms live coiled together inside lymphatic vessels for up to 7 years!
04 — HISTORICAL TIMELINE
~600 BCE
Ancient Records
Hindu texts describe elephantiasis-like swelling. Ancient Egyptians also recorded the disease.
1863
Discovery
Jean-Nicolas Demarquay discovers microfilaria in lymphatic fluid. Timothy Lewis finds microfilaria in blood.
1877
Worm Identified
Joseph Bancroft discovers adult Wuchereria bancrofti worm in Australia.
1878
Mosquito Link
Patrick Manson proves mosquitoes transmit the parasite — first insect-disease transmission proven in history!
1900s
Naming
Disease officially named Wuchereria bancrofti after Wucherer & Bancroft.
1947
DEC Treatment
Diethylcarbamazine (DEC) developed as first effective drug treatment.
2000
WHO GPELF
Global Programme to Eliminate Lymphatic Filariasis launched. Mass drug administration begins worldwide.
2024
Progress
21 countries achieve elimination status. 69% reduction in global burden.
Patrick Manson's 1878 discovery was a landmark moment — it was the FIRST proof that insects can transmit human disease.
06 — INCUBATION PERIOD & SYMPTOMS
6–12
MONTHS
Incubation Period
Time between mosquito bite and first symptoms
Microfilariae may circulate in blood for <strong style="font-weight: 800; color: #fff; background-color: rgba(26, 74, 46, 0.4); padding: 0 8px; border-radius: 4px;">MONTHS</strong> before symptoms appear
Many people remain asymptomatic despite being infected
Adult worms take months to mature in lymphatic vessels
Acute Stage
<strong style="color: #f97316;">Lymphangitis</strong> (inflamed lymph vessels)
<strong style="color: #f97316;">Lymphadenitis</strong> (swollen lymph nodes)
Recurring fever and chills
Pain and tenderness
Elevated eosinophils in blood
Chronic Stage (years later)
<strong style="color: #10b981;">Lymphedema</strong> — massive swelling of limbs
<strong style="color: #10b981;">Elephantiasis</strong> — thickened, rough "elephant skin"
<strong style="color: #10b981;">Hydrocele</strong> — fluid in scrotum (males)
<strong style="color: #10b981;">Chyluria</strong> — milky white urine
Breast/genital swelling
Most infected people never show visible symptoms — but lymphatic damage occurs silently inside the body.
07 — RISK FACTORS & COMPLICATIONS
⚠️ RISK FACTORS
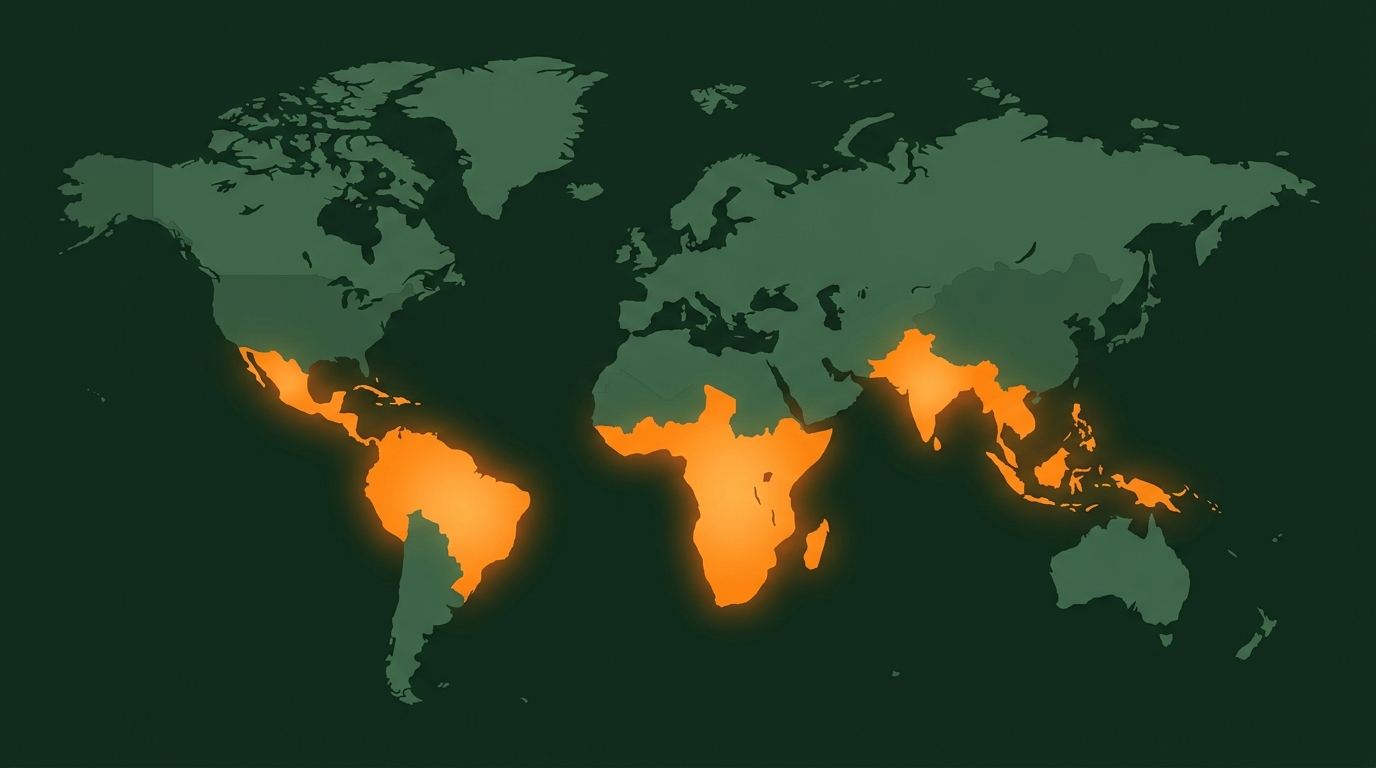
Living in endemic tropical/subtropical regions (Africa, Asia, Pacific)
High mosquito exposure — poor housing, no nets
Lack of clean water & sanitation
Sleeping without mosquito protection
Long-term residence since childhood in endemic area
Limited access to healthcare/treatment
🚨 POTENTIAL COMPLICATIONS
Permanent Lymphedema
Irreversible swelling of limbs, causing lifelong disability
Elephantiasis
Gross enlargement of limbs/genitals; skin becomes thick, warty, darkened
Hydrocele
Accumulation of fluid around the testes; affects up to 25% of males in endemic areas
Secondary bacterial infections
Repeated skin infections due to damaged lymphatic defenses
Psychological & Social Impact
Stigma, depression, inability to work; major disability burden
Elephantiasis causes ~1.31 million DALYs (disability-adjusted life years) lost globally each year — it is a leading cause of permanent disability.
08 — TREATMENT & MANAGEMENT
DRUG OF CHOICE
Diethylcarbamazine (DEC)
MICROFILARICIDE
Ivermectin
COMBINATION THERAPY
Albendazole
Lymphedema Management
Surgical Options
09 — VACCINATION & CONTROL PROGRAMS
NO VACCINE EXISTS
There is currently no approved vaccine for Lymphatic Filariasis. Prevention relies on drug treatment and mosquito control.
WHO Global Programme (GPELF)
Est. 2000
Mass Drug Administration (MDA)
Vector (Mosquito) Control
37
Countries no longer need MDA
924M
People free from required treatment
69%
Reduction in global burden achieved
~57 MILLION
People infected globally (2021)
1.31 MILLION
DALYs lost per year (disability burden)
72 COUNTRIES
Endemic nations worldwide
10+ BILLION
Treatments delivered since 2000
11 — IMAGES OF THE PATHOGEN & DISEASE
Wuchereria bancrofti microfilaria under light microscopy (CDC)
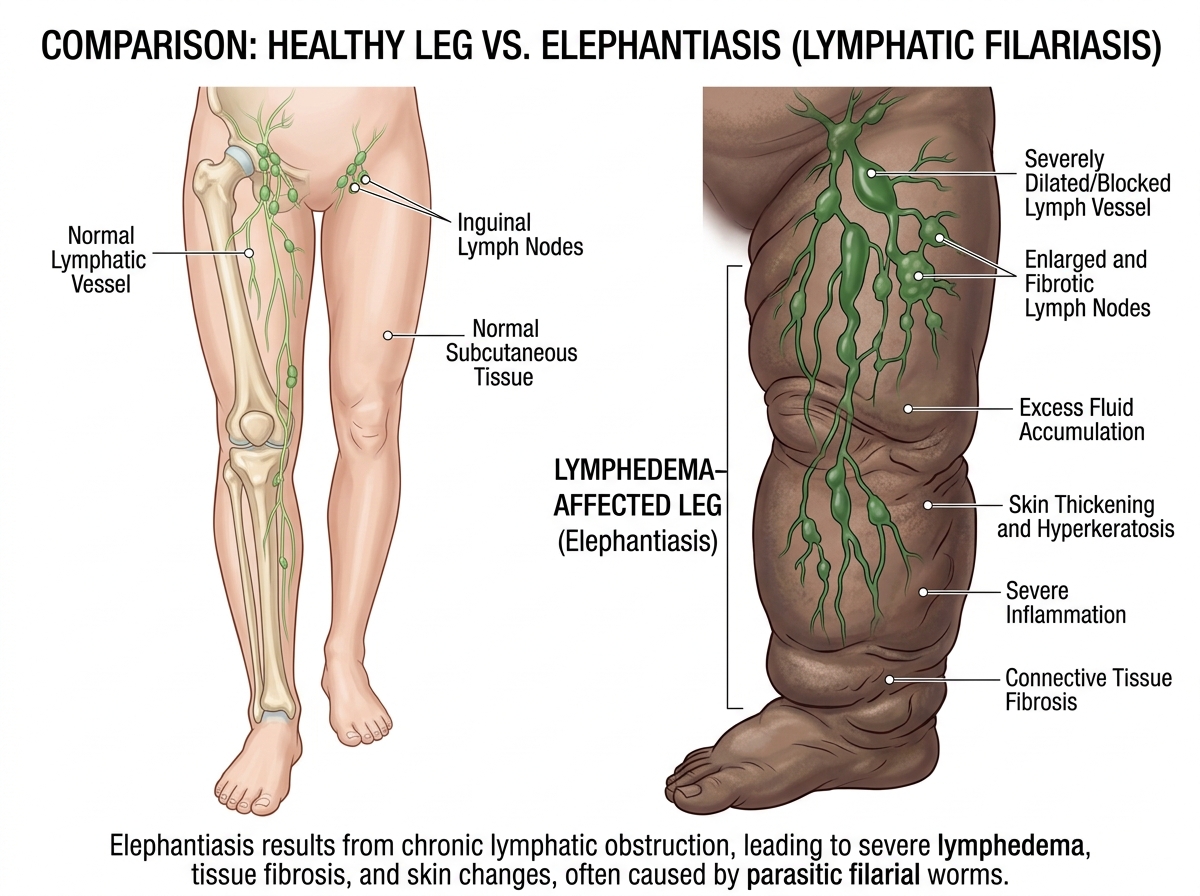
Elephantiasis: severe lymphedema of the leg
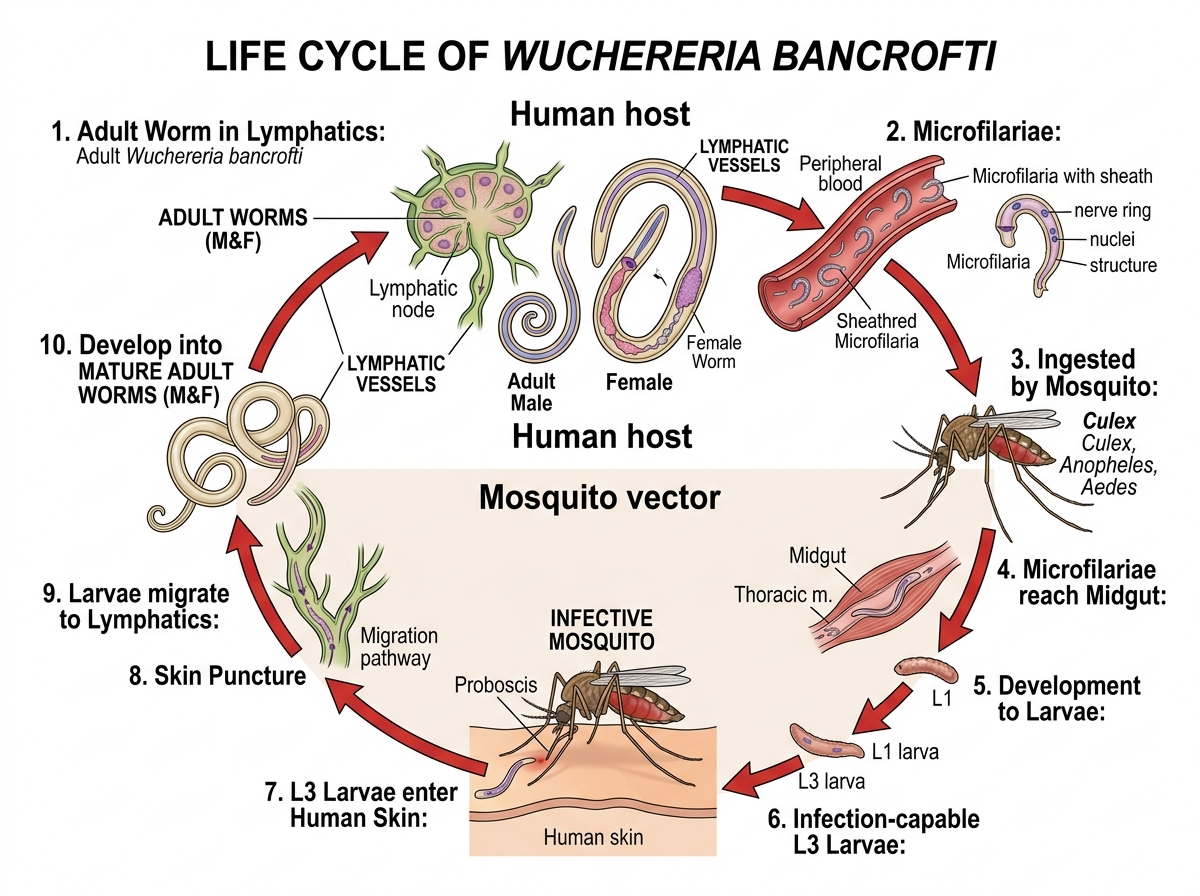
Life Cycle of W. bancrofti
Culex quinquefasciatus — main vector mosquito
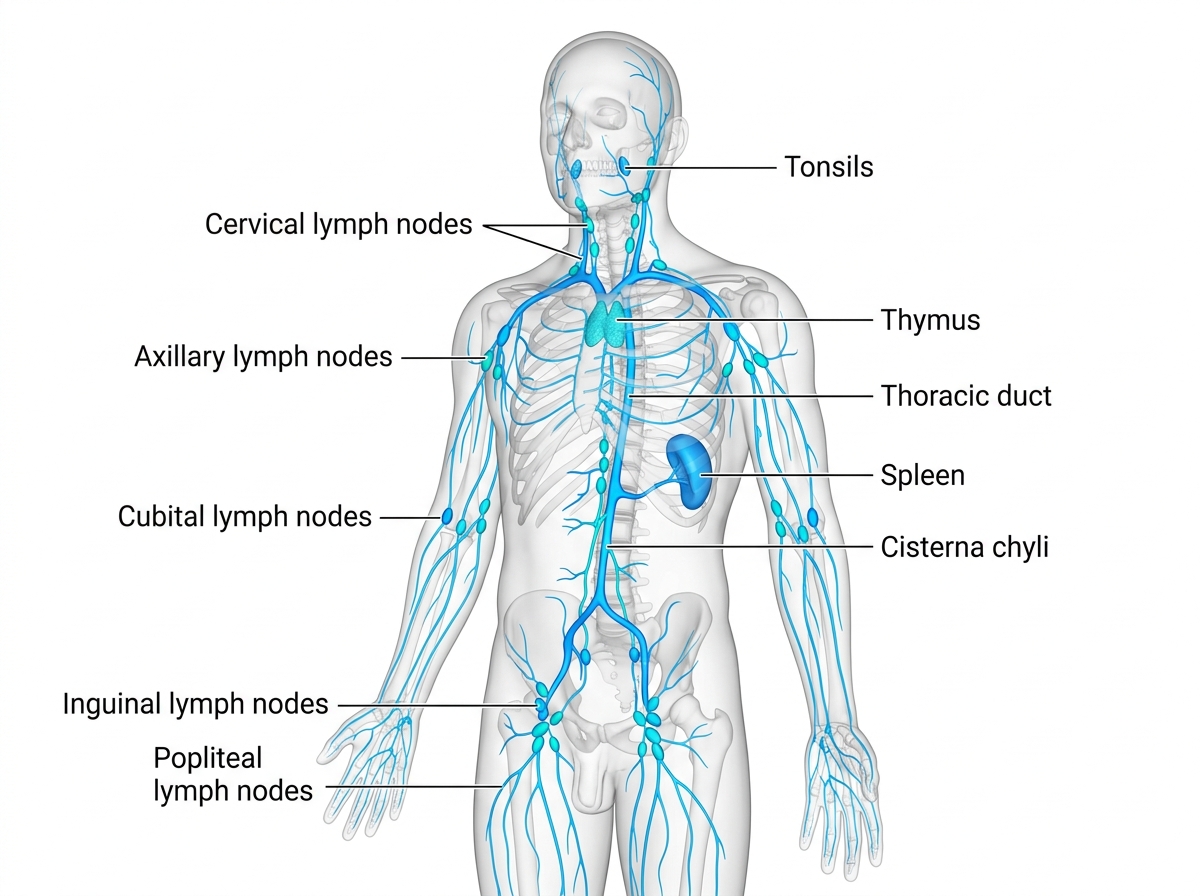
Human lymphatic system affected by LF
KEY TAKEAWAYS
🦟
Spread by mosquito bites — NOT person to person
🪱
Caused by Wuchereria bancrofti — a parasitic roundworm
⏱️
6–12 month incubation — silent damage inside body
💊
Treatable with DEC, Ivermectin & Albendazole (IDA)
🌍
~57 million infected — a Neglected Tropical Disease
✅
Eliminatable! 21 countries already disease-free (2024)
Elephantiasis is PREVENTABLE, TREATABLE & ELIMINATABLE — with the right tools and global commitment.
Sources: WHO, CDC, Global Burden of Disease Study 2021
- elephantiasis
- lymphatic-filariasis
- infectious-disease
- tropical-medicine
- wuchereria-bancrofti
- parasitology
- global-health