Biopsychosocial Approach to Complex Mental Health Risk
Learn how to manage mental health risk in people with complex physical and psychological conditions using a trauma-informed, biopsychosocial approach.
Managing Mental Health Risk in People with Complex Conditions
A Biopsychosocial, Trauma-Informed Approach
Course Overview
<ul><li>Interaction of co-existing physical & mental health conditions</li><li>Impact on distress, vulnerability, and risk</li><li>Risk identification & management</li><li>Therapeutic engagement strategies</li><li>Legal frameworks (MHA & MCA)</li><li>Person-centred, least restrictive care</li></ul>
Course Aims
<ul><li>Understand impact of physical illness on mental health</li><li>Identify risk factors using biopsychosocial approach</li><li>Promote safety, dignity, and recovery</li><li>Apply legal and safeguarding frameworks confidently</li></ul>
Physical Health Conditions & Mental Health
Fibromyalgia
CNS sensitisation & chronic pain. Impacts mood, sleep, cognition, and emotional regulation.
PCOS
Hormonal imbalance affecting mood, self-esteem, and anxiety levels.
Endometriosis
Chronic pain leading to depression, trauma responses, and reduced quality of life.
Additional Physical Conditions
<ul><li><strong>Non-Allergic Rhinitis:</strong> Chronic symptoms causing fatigue and sleep disturbance.</li><li><strong>Migraines:</strong> Neurological condition linked with anxiety, avoidance, and depression.</li><li><strong>Ehlers-Danlos Syndrome (EDS):</strong> Chronic pain, fatigue, autonomic dysfunction.</li></ul>
Mental Health & Neurodevelopmental Conditions
<ul><li><strong>Depression & Anxiety Disorders:</strong> Common comorbidities that amplify physical symptoms.</li><li><strong>ADHD:</strong> Impacts executive functioning and impulsivity.</li><li><strong>Complex PTSD:</strong> Involves trauma, hypervigilance, and emotional dysregulation.</li><li><strong>EUPD / Borderline Personality Disorder:</strong> Challenges with emotional regulation and relationships.</li></ul>
Key Point: Physical and mental health conditions interact and amplify risk.
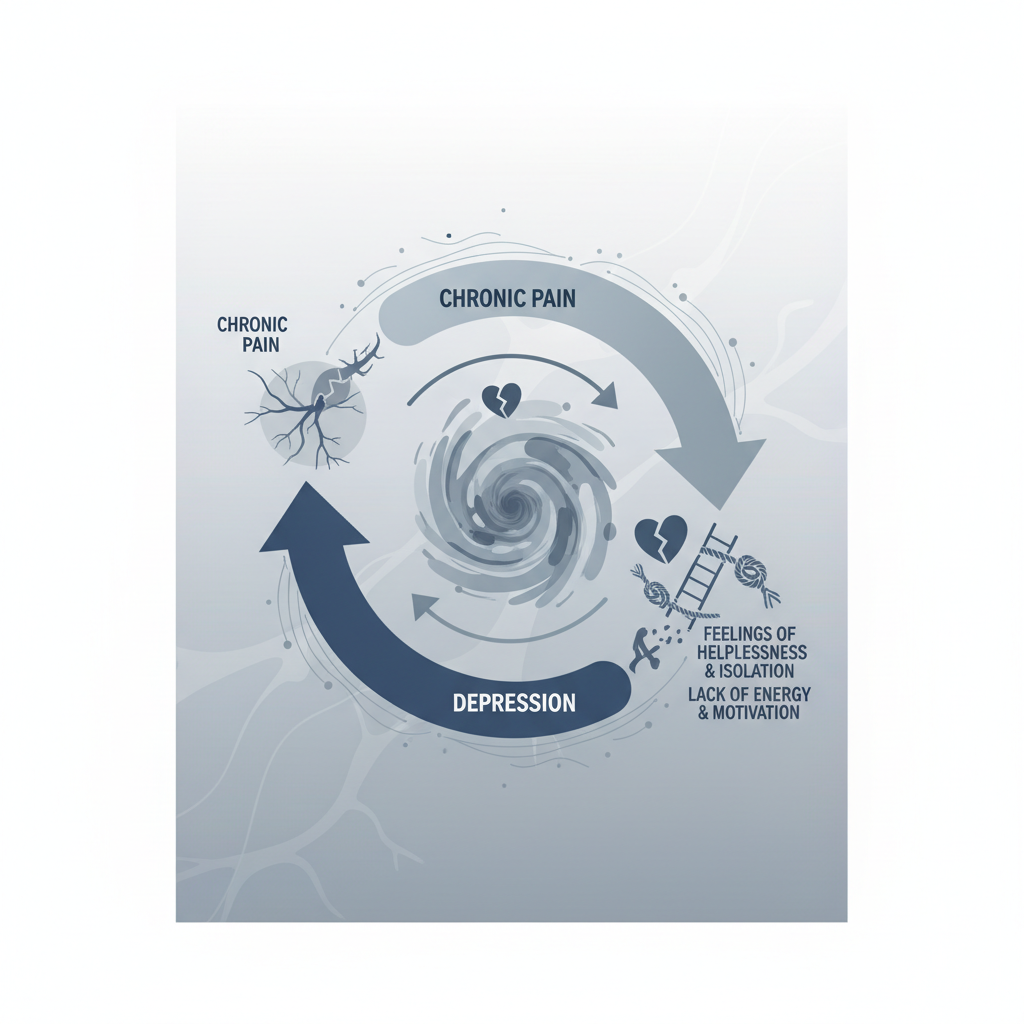
Depression & Anxiety in Complex Care
<ul><li><strong>The Pain-Depression Cycle:</strong> Chronic pain depletes serotonin and dopamine, worsening mood.</li><li><strong>Hopelessness:</strong> Pain limits activity, leading to isolation and reduced quality of life.</li><li><strong>Anxiety & Panic:</strong> Physical symptoms (palpitations, breathlessness) often mimic cardiac events.</li><li><strong>Impact on Care:</strong> Reduced motivation for rehab or self-care routines.</li></ul>
Key Point: Treating physical symptoms without addressing mood often leads to poor outcomes.
Neurodevelopmental Conditions (ADHD & Autism)
<ul><li><strong>Executive Dysfunction:</strong> Difficulties with planning, initiating tasks, or managing medication schedules.</li><li><strong>Sensory Needs:</strong> Bright lights, noise, or touch can be overwhelming or painful.</li><li><strong>Communication:</strong> May need literal, unambiguous instructions; metaphors can be confusing.</li><li><strong>Impulsivity:</strong> Increased risk of rapid decision-making or emotional reactivity.</li></ul>
Key Point: Adjusting the environment and communication style is vital for effective engagement.
Complex Trauma & EUPD
<ul><li><strong>Emotional Dysregulation:</strong> Intense emotions that are difficult to soothe without support.</li><li><strong>Hypervigilance:</strong> Constant scanning for threat; high state of physiological arousal.</li><li><strong>Relational Challenges:</strong> Difficulty with trust; fear of abandonment vs rejection sensitivity.</li><li><strong>Internal Experience:</strong> Distress may be masked ("Quiet BPD") or expressed via self-harm.</li></ul>
Key Point: Consistency, reliability, and clear boundaries are the foundations of safety.
Maintaining & Managing Conditions
<ul><li><strong>Pain Management & Pacing:</strong> Crucial for physical stability.</li><li><strong>Psychological Support:</strong> CBT, grounding techniques, and mindfulness.</li><li><strong>Sleep Hygiene:</strong> Addressing sleep disturbance to improve mood.</li><li><strong>Medication Review:</strong> Regular monitoring for side effects and efficacy.</li><li><strong>MDT Input:</strong> Collaborative care involving all specialists.</li><li><strong>Validation:</strong> Acknowledging lived experience reduces distress.</li></ul>
Depression & Anxiety in Complex Care
<ul><li><strong>Depression:</strong> Often linked to chronic pain and loss of function. Reduces motivation for self-care.</li><li><strong>Anxiety:</strong> Panic attacks can mimic physical emergencies (e.g., cardiac issues).</li><li><strong>Impact:</strong> Both conditions increase pain perception and reduce the threshold for coping.</li></ul>
Risk: Hopelessness increases the risk of self-neglect and suicide.
Neurodevelopmental Conditions (ADHD & Autism)
<ul><li><strong>Executive Dysfunction:</strong> Difficulty planning, remembering appointments, or organizing medication.</li><li><strong>Sensory Sensitivity:</strong> Hospital lights, noise, and touch can cause severe distress or 'meltdowns'.</li><li><strong>Impulsivity:</strong> Higher risk of self-discharge or substance misuse as coping mechanisms.</li></ul>
Risk: 'Non-compliance' is often actually executive dysfunction or sensory overwhelm.
Complex Trauma & EUPD
<ul><li><strong>Emotional Dysregulation:</strong> Intense emotional pain triggered by physical symptoms or perceived rejection.</li><li><strong>Trust Issues:</strong> Previous trauma (medical or interpersonal) makes trusting staff difficult.</li><li><strong>Hypervigilance:</strong> Constant state of alert can worsen chronic pain and fatigue.</li></ul>
Risk: Self-harm may be used to regulate overwhelming distress.
Case Application: Chronic Pain & Risk
Sarah (45) has a diagnosis of Fibromyalgia. She is currently in a severe flare-up, hasn't slept in 3 days, and expresses that she 'cannot go on like this'.
<ul><li>How might sleep deprivation impact her immediate suicide risk?</li><li>What physiological factors (pain, fatigue) are acting as drivers for her distress?</li><li>How would you validate her pain while assessing safety?</li></ul>
The Biopsychosocial Model of Risk
Biological (Physical)
Pain, Infection, Delirium, Medication Side Effects, Hypoglycaemia.
Psychological
Trauma, Grief, Cognitive Impairment, Coping Skills.
Social
Isolation, Financial stress, Housing, Support networks.
Therapeutic Observation
Primary Purpose: Maintain safety, reduce harm, support recovery.
<ul><li><strong>General:</strong> Hourly checks (Low risk)</li><li><strong>Intermittent:</strong> Every 15 mins, unpredictable (Potential risk)</li><li><strong>Eyesight:</strong> Always seen (High risk)</li><li><strong>Arm’s Length:</strong> Close proximity (Immediate risk)</li></ul>
Case Application: Delirium vs Behaviour
Elsie (78) is usually successfully supported at home. Suddenly, she becomes aggressive, confused, and paranoid about carers 'stealing'.
<ul><li>Before assuming a mental health relapse, what physical causes must be ruled out? (e.g., UTI, dehydration)</li><li>How does the 'Least Restrictive' principle apply here?</li><li>Why is therapeutic observation critical during this assessment phase?</li></ul>
Building Therapeutic Relationships
<ul><li><strong>Empathy & Compassion:</strong> Foundational for trust.</li><li><strong>Active Listening:</strong> Listen to understand, not just to respond.</li><li><strong>Calm Communication:</strong> De-escalates anxiety.</li><li><strong>Trauma-Informed:</strong> 'What happened to you?' not 'What is wrong with you?'</li><li><strong>Consistency:</strong> Reliability builds safety.</li></ul>
Supporting Self-Neglect
<ul><li>Avoid judgement or pressure.</li><li>Break tasks into small, manageable steps.</li><li>Offer choices to restore a sense of control.</li><li>Validate the distress underlying the neglect.</li><li>Graded exposure: Gradual re-engagement with care tasks.</li></ul>
Legal Frameworks: MHA vs MCA
Mental Health Act (MHA)
Used when risk is linked to mental disorder.<br>Allows compulsory assessment/treatment.<br>Specific to mental health treatment.
Mental Capacity Act (MCA)
Used when decision-making capacity is impaired.<br>Best Interests decisions.<br>Applies to physical health & care decisions.
Trauma-Informed Language
<table style='width:100%; border-collapse:collapse; font-size:24px;'><thead><tr style='background-color:#005691; color:white;'><th style='padding:15px; text-align:left;'>Instead of (Negative)</th><th style='padding:15px; text-align:left;'>Try (Positive/Informed)</th></tr></thead><tbody><tr style='background-color:#F0F4F8;'><td style='padding:15px; border-bottom:1px solid #ccc;'>Calm down</td><td style='padding:15px; border-bottom:1px solid #ccc;'>Try and relax</td></tr><tr style='background-color:#fff;'><td style='padding:15px; border-bottom:1px solid #ccc;'>You have to...</td><td style='padding:15px; border-bottom:1px solid #ccc;'>Can we try... / Shall we...</td></tr><tr style='background-color:#F0F4F8;'><td style='padding:15px; border-bottom:1px solid #ccc;'>Kicking off</td><td style='padding:15px; border-bottom:1px solid #ccc;'>Presenting with distress</td></tr><tr style='background-color:#fff;'><td style='padding:15px; border-bottom:1px solid #ccc;'>Non-compliant</td><td style='padding:15px; border-bottom:1px solid #ccc;'>Not in agreement / Declining</td></tr><tr style='background-color:#F0F4F8;'><td style='padding:15px; border-bottom:1px solid #ccc;'>Paranoid</td><td style='padding:15px; border-bottom:1px solid #ccc;'>Experiencing unusual thoughts</td></tr></tbody></table>
Course Outcome
Participants can now:<br>• Promote safety<br>• Reduce risk<br>• Support recovery<br>• Enable meaningful lives
- trauma-informed
- biopsychosocial-model
- mental-health-risk
- person-centred-care
- healthcare-training
- complex-conditions
- legal-frameworks