Technological Advances in Interventional Radiology: AI & Robotics
Explore how AI, Robotics, Extended Reality (XR), and CBCT imaging are transforming Interventional Radiology into a safer, more precise medical field.
Medical Student Overview
Technological Advances in Interventional Radiology
AI • Robotics • Extended Reality • CBCT Imaging
A Review of Modern IR Innovations
Introduction
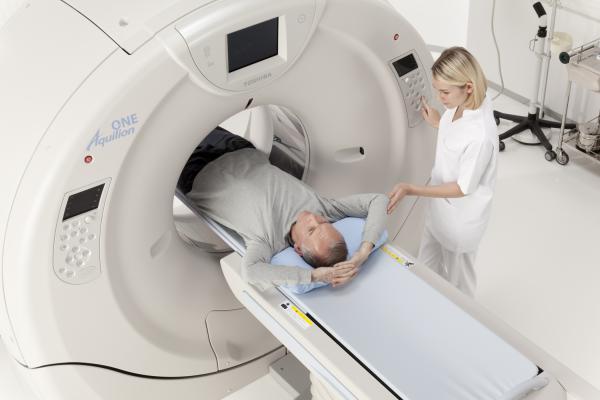
What is Interventional Radiology?
Minimally invasive procedures guided by medical imaging
Combines diagnostic imaging with targeted therapy
Alternative to open and laparoscopic surgery
Shorter hospital stays, faster recovery, less pain
Global IR market valued at ~USD $25–30 billion in the mid-2020s, projected to keep growing through 2030
Agenda
What We'll Cover Today
01 — CBCT & Image Fusion
Real-time 3D imaging inside the procedure room
02 — Artificial Intelligence
Smarter planning, guidance & outcome prediction
03 — Extended Reality (XR)
Training, planning & AR-guided procedures
04 — Robotics in IR
Precision, safety & remote interventions
Plus: Ethics, challenges & future directions
CBCT & Imaging
Cone-Beam CT: Seeing in 3D During the Procedure
What is it?
A C-arm rotates around the patient and reconstructs a full 3D image in under 20 seconds — right there in the procedure room.
Why does it matter?
Real-time 3D visualisation — no CT scanner trip needed
Overlay tumour maps and vessel roadmaps onto live fluoroscopy
Improves needle and catheter placement accuracy
Think of it as:
A CT scanner built into your procedure suite
CBCT Clinical Benefits
Where CBCT Makes a Real Difference
Systematic review showed improved 1-year local progression-free survival & 3-year overall survival with CBCT-guided TACE vs conventional guidance
Artificial Intelligence
AI in IR: Smarter Medicine
AI in IR includes machine learning, deep learning (neural networks), and large language models — used across the entire procedural workflow.
BEFORE the procedure
Patient selection, outcome prediction, procedural planning
DURING the procedure
Image enhancement, device tracking, real-time navigation guidance
AFTER the procedure
Complication detection, treatment response evaluation
Most AI tools are decision-support — the doctor is still in charge ✅
AI: Clinical Impact
What Can AI Actually Do in IR?
Predicting Treatment Response
In liver cancer (HCC) treated with TACE:
Combines imaging features + clinical data
AUC of ~0.75–0.85 for predicting response
Helps avoid non-beneficial procedures
Like a data-backed second opinion
Radiation and Image Quality
During the procedure:
AI reduces fluoroscopy radiation dose
Noise suppression improves image clarity
Real-time catheter and device tracking
Less radiation, better images
Extended Reality (XR)
AR, VR & MR: Reality Gets an Upgrade
Extended Reality = a spectrum of technologies that blend real and digital worlds
Virtual Reality (VR)
Fully immersive digital environment — replaces the real world
🎓 Training & simulation — practice procedures without real patients
30–50% reduction in fluoroscopy time during simulated tasks
Augmented Reality (AR)
Digital content overlaid onto the real world in real-time
🎯 Live procedure guidance — overlay vessel maps & needle paths
Accurate target access with holographic needle guidance
Mixed Reality (MR)
Interactive blending of real and digital with spatial awareness
📐 Collaborative 3D planning before complex procedures
Reduces contrast use and imaging requirements
XR: Clinical Benefits
XR in Practice: Training to Theatre
TRAINING
VR simulators improve technical performance vs conventional training — most useful for early trainees
30–50% less fluoroscopy time in simulated tasks
<svg xmlns="http://www.w3.org/2000/svg" width="36" height="36" viewBox="0 0 24 24" fill="none" stroke="currentColor" stroke-width="2.5" stroke-linecap="round" stroke-linejoin="round"><path d="M22 10v6M2 10l10-5 10 5-10 5z"/><path d="M6 12v5c3 3 9 3 12 0v-5"/></svg>
PROCEDURAL GUIDANCE
AR/MR overlays used for vertebroplasty, biopsies, ablations — holographic needle guidance on real patient
Sub-millimetric to low-mm targeting accuracy in phantom studies
<svg xmlns="http://www.w3.org/2000/svg" width="36" height="36" viewBox="0 0 24 24" fill="none" stroke="currentColor" stroke-width="2.5" stroke-linecap="round" stroke-linejoin="round"><circle cx="12" cy="12" r="10"/><circle cx="12" cy="12" r="6"/><circle cx="12" cy="12" r="2"/></svg>
RADIATION REDUCTION
XR-guided spine/percutaneous procedures → meaningful reduction in fluoroscopy dose
Some series: ~50% dose reduction vs conventional workflows
<svg xmlns="http://www.w3.org/2000/svg" width="36" height="36" viewBox="0 0 24 24" fill="none" stroke="currentColor" stroke-width="2.5" stroke-linecap="round" stroke-linejoin="round"><path d="M12 22s8-4 8-10V5l-8-3-8 3v7c0 6 8 10 8 10z"/><polyline points="8 12 12 16 16 12"/><line x1="12" y1="8" x2="12" y2="16"/></svg>
Robotics in IR
Robots in the Angiography Suite
Robotic systems translate joystick/console inputs into precise millimetric movements of guidewires and catheters — operator works from a shielded control station.
Endovascular Robots
Remote manipulation of guidewires & catheters
Used in: cerebral aneurysm embolisation, peripheral arterial disease, complex aortic repair
Primary effectiveness >90% in neurovascular trials
Percutaneous Robots
CT/MRI/ultrasound-guided needle placement
Standardises insertion angles & depths
Sub-millimetric targeting accuracy in phantom studies
Robotics: Key Benefits
Why Use Robots? Safety, Precision & Beyond
Radiation Protection
Operators work from a shielded remote workstation — drastically cutting their radiation dose during complex procedures.
80–90% reduction in operator radiation dose vs conventional techniques
Ergonomics & Health
Reduces musculoskeletal strain from prolonged procedure positions. Addresses a well-known occupational hazard in IR.
Improved operator comfort & reduced physical fatigue
Remote & Tele-Intervention
Experimental remote procedures over secure networks — could bring specialist IR care to remote or underserved regions.
Technical feasibility demonstrated — regulatory challenges remain
Patient radiation exposure: comparable to or modestly reduced vs conventional approaches when optimised
Challenges & Costs
Innovation Comes at a Price
CBCT Systems
💰 Mid-6 to low-7 figure range (hardware + suite build-out)
May be offset by fewer repeat procedures & shorter hospital stays in high-volume centres
AI Tools
💰 Varies — software licensing, infrastructure
Limited IR-specific economic data; workflow integration & validation still needed
XR Hardware
💰 Several thousand to low 5-figure USD
Lack of standardisation, ergonomic limitations, infection control considerations
Robotic Systems
💰 High 6-figure range + ongoing maintenance
Limited haptic feedback, device compatibility issues, small number of centres currently using
⚖️ Well-resourced vs resource-limited settings — risk of widening healthcare inequity
🔮 As volumes increase & competition grows → costs expected to fall over time
Ethics
With Great Technology Comes Great Responsibility
Data Privacy
Patient imaging data used to train AI must be protected — de-identified data still carries re-identification risk
Algorithmic Bias
AI trained on non-diverse datasets may underperform in certain populations — could worsen health inequities
Transparency
Doctors must understand how AI recommendations are generated — black box models are problematic
Accountability
The interventional radiologist retains ultimate responsibility — AI is a tool, not the doctor
Informed Consent
Patients should know when advanced technologies guide their procedures
Equity & Access
Advanced tech risks widening gaps between well-resourced and resource-limited healthcare systems
Key principle: AI/XR/Robotics = Decision SUPPORT tools under human oversight — not autonomous operators
The Future of IR
Convergence: When All Technologies Work Together
The next phase of IR combines CBCT, AI, XR and Robotics into unified procedural systems
AI modules for path planning and real-time optimisation built into robotic control systems
XR overlays delivering live 3D anatomy into the operator's field during robotic procedures
Tele-interventional hubs enabling remote specialist procedures in underserved regions
Ultra-low-dose protocols to expand access in resource-limited settings
Multicentre trials, standardised reporting, cost-effectiveness analyses, and robust ethical governance
Summary
Key Takeaways for Medical Students
1
IR is minimally invasive medicine guided by imaging
Fewer complications, shorter stays, faster recovery than open surgery
2
CBCT gives real-time 3D vision inside the procedure room
Improves accuracy for liver, bone, vascular, and spinal interventions
3
AI supports decisions — it does not replace the doctor
Predicts outcomes, improves images, and automates documentation
4
XR trains the next generation and guides complex cases
VR for simulation, AR/MR for live holographic guidance
5
Robotics protects operators and expands what is possible
80–90% less radiation for the operator; future potential for remote care
The future: CBCT + AI + XR + Robotics = safer, smarter, more accessible interventional care
Thank You
Questions & Discussion
Technological Advances in Interventional Radiology
Based on: Modern IR Advances — Narrative Review, 2025
CBCT & Imaging • Artificial Intelligence • Extended Reality • Robotics
- interventional-radiology
- medical-technology
- artificial-intelligence
- robotics
- extended-reality
- cbct-imaging
- medical-education