Managing Post-Chemotherapy Refractory Diarrhea & Colitis
Exploration of clinical challenges in refractory diarrhea post-chemotherapy, covering C. difficile, pembrolizumab-induced colitis (irAE), and CMV colitis.
A Multi-Hit Diagnostic Dilemma: Refractory Diarrhea Post-Chemotherapy
Navigating C. difficile, Pembrolizumab-Induced Colitis (irAE), and Opportunistic Infections
Framework: Based on UKONS, CCO, and BC Cancer Toxicity Management Standards
Presenter: [Your Name]
Clinical Presentation & History
Patient: Middle-aged female, Breast Cancer
Timeline: Day +10 post-chemotherapy (recent Pembrolizumab exposure)
Admission Symptoms: Nausea, vomiting, abdominal pain, and profuse non-bloody diarrhea (18-22 episodes/day)
Initial Observations: Tachycardia (Fast Atrial Fibrillation), otherwise stable
Initial Investigations & Toxicity Grading
Laboratory Findings: CRP >400 mg/L, AKI Stage 2, Low K+ and Mg2+
CTCAE v5.0 Grading (CCO/BC Cancer)
Grade 3 Colitis: Increase of ≥ 7 stools over baseline; incontinence; hospitalization required.
Management: IV Ceftazidime (Neutropenic sepsis cover per UKONS), fluid resuscitation, electrolyte replacement.
Status: AKI and AF resolved. CRP began trending down.
The 'Toxin-Negative' Diagnostic Gap
Microbiology: C. diff PCR (+), but Toxin (–) on multiple samples.
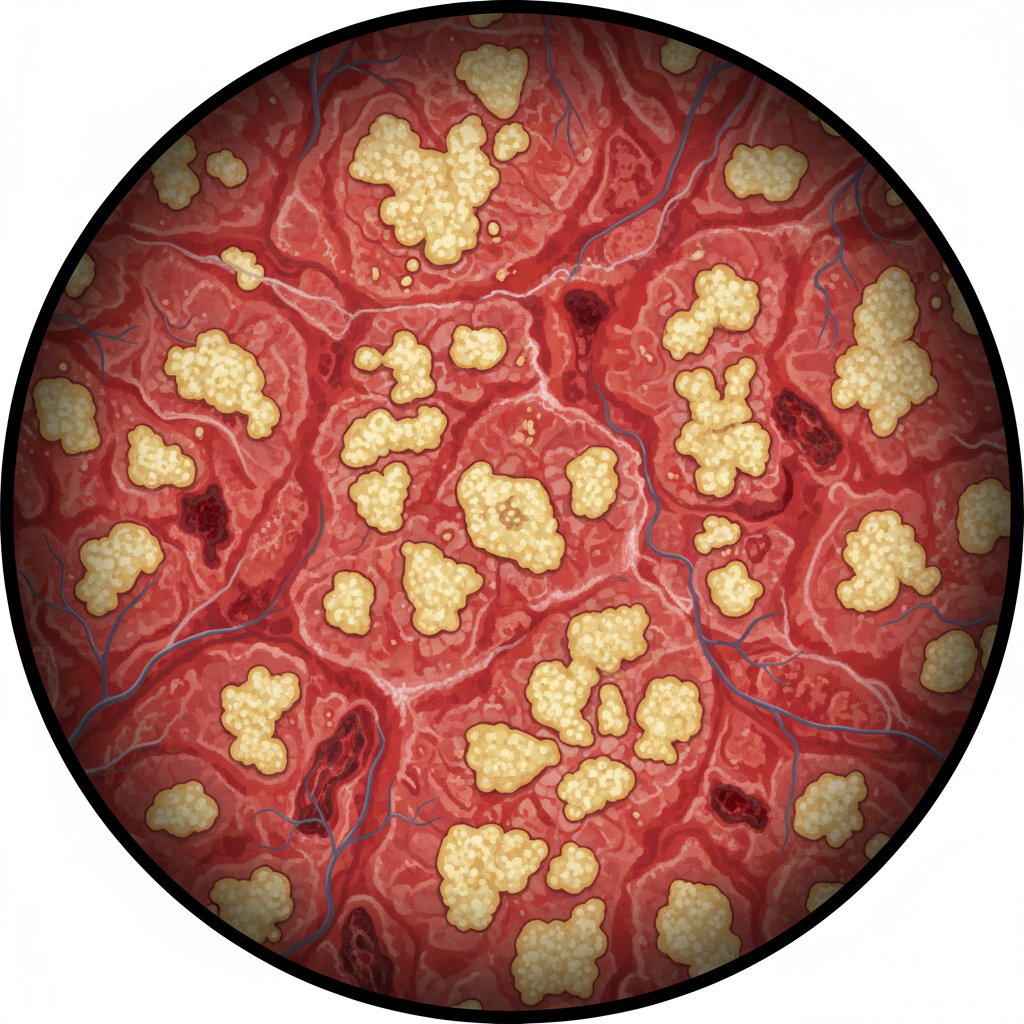
Endoscopy: Pseudomembranous Colitis confirmed on flexible sigmoidoscopy.
Clinical Insight: BC Cancer/CCO guidelines state that visual pseudomembranes supersede negative toxin assays.
Intervention: High-dose Oral Vancomycin (250mg Q4H) and IV Metronidazole.
Differential 1: Refractory C. difficile
Definition: Persistent symptoms after 10+ days of therapy.
Mechanism of Failure: Potential 'Toxin Dilution' due to ultra-high output (20+ stools/day).
Escalation: Fecal Microbiota Transplant (FMT) consideration to restore the microbiome barrier.
Differential 2: Pembrolizumab-Induced Colitis
Mechanism: PD-1 inhibition leads to T-cell mediated attack on colonic mucosa.
The 'Double-Hit' Hypothesis: Chemotherapy-induced mucosal injury likely allowed Pembrolizumab-activated T-cells to aggressively infiltrate the tissue.
Histology Targets: Crypt Epithelial Cell Apoptosis and intense lymphocytic infiltration (distinct from 'Volcano' lesions typical of CDI).
Differential 3: CMV Colitis
Context: Opportunistic reactivation in immunocompromised oncology patients.
Status: Weakly positive CMV IgM; CMV DNA PCR (Viral Load) pending.
BC Cancer Caveat: Mandatory rule-out of CMV before starting high-dose steroids for irAEs to prevent bowel perforation.
The Clinical Paradox: CRP vs. Symptoms
Clinical Interpretation
Systemic infection (Sepsis) is suppressed.
Infectious Driver likely replaced by Immune-Mediated Organ Failure.
Normal CRP makes steroid initiation safer (reduced sepsis risk).
Management Algorithm (Integrated Standards)
1. Rule Out CMV
Confirm negative blood PCR before introducing immunosuppression.
2. Restore Microbiome
Prioritize FMT for refractory C. diff presentations.
3. The Transition (CCO/BC Cancer)
Initiate IV Methylprednisolone 1-2 mg/kg. If refractory >48h: Escalate to Infliximab or Vedolizumab.
Nursing & Supportive Care (UKONS Focus)
UKONS 24-Hour Triage: Patient remains in 'Red/Amber' category due to stool volume.
Electrolyte Management: Strict monitoring of K+ and Mg2+ to prevent recurrence of AF.
Skin Integrity: Proactive management of perianal skin breakdown due to high-frequency output.
Consolidated Reference Links
UK Oncology Nursing Society (UKONS): 24-Hour Triage Tool
Cancer Care Ontario (CCO): Immune Checkpoint Inhibitor Toolkit
BC Cancer: Management of ICI Toxicities (Section 15.6)
IDSA: 2021 C. Difficile Management Update
Discussion & Next Steps
Immediate Actions
Await CMV PCR Viral Load results. Finalize Micro/Gastro review for potential Fecal Microbiota Transplant (FMT).
The Clinical Question
Given the normal CRP, should we proceed with a steroid trial if FMT does not yield a rapid response?
- oncology
- chemotherapy-side-effects
- immunotherapy-toxicities
- c-difficile
- clinical-case-study
- pembrolizumab
- medical-education